Dermal Oncoimmunology Junior Group
Dr. Hafsa Munir
Manipulating cancer-associated fibroblasts to favour a robust anti-tumor immune response
OUR RESEARCH
Why it matters
While huge leaps have been made to improve the detection, prevention, and treatment of skin cancer, the overall incidence has increased over the past 10 years, which is due in part to the climate crisis. Cutaneous melanoma comprises only 2% of all skin cancers but contributes to more than 80% of skin cancer-related deaths. Despite the success of immune checkpoint inhibitors for treating melanoma, 40-70% of patients develop resistance. Stromal cells in the skin can induce resistance to multiple cancer therapies and therefore are an attractive target for cancer therapy. The Dermal Oncoimmunology Lab aims to identify stromal mediated mechanisms of resistance and devise ways of modifying the state of the stromal cells to overcome therapeutic resistance.
MUNIR LAB
Lab focus
Cancers are a highly heterogenous group of diseases. This diversity is not restricted to the malignant cells, but rather extends to the surrounding microenvironment (ME; containing fibroblasts, endothelial cells and immune cells). Recent work has shown that the state of the tumour ME plays a significant role on the anti-tumour immune response and sensitivity to immune-checkpoint inhibitors.
While autoimmune disease and cancer are opposing conditions, both are indisputably interconnected. Indeed, both are chronic inflammatory conditions in which the ME regulates disease progression through effects exerted on immune cells. Additionally, the advent of therapeutic agents targeting immune checkpoints and that autoimmunity in cancer is a positive prognostic marker highlight how inducing an autoimmune-like state within tumours could be pivotal for developing novel ways to treat cancer.
Cancer-associated fibroblasts (CAFs) provide an attractive target for driving an autoimmune-like state in tumours as these cells are critical regulators of the immune response. In the Dermal Oncoimmunology lab, we place fibroblasts at the centre of immune-regulatory networks in the skin during autoimmunity and cancer. We strive to elucidate and compare the phenotype and function of subsets of skin CAFs with those from autoimmune skin lesions. In turn, we will manipulate the CAFs to mimic aspects of fibroblasts from autoimmune skin lesions to favour a robust anti-tumour immune response.
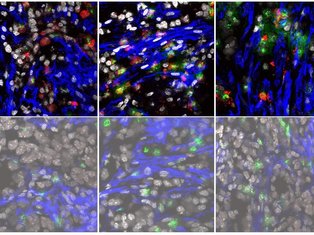
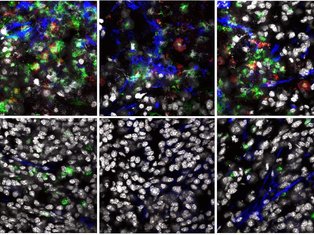
Our lab will combine multiplexed flow cytometry, confocal microscopy with single-cell sequencing and spatial transcriptomics to characterise the phenotype and function of fibroblasts and infiltrating immune cells in the skin of patients with cancer or autoimmune skin lesions. We will also use advanced imaging tools to assess tissue topography and location of fibroblast subsets in these conditions.
We will develop and utilise microfluidic platforms incorporating complex3D multicellular matrices, organotypic cultures and novel in vitro approaches to dissect the fibroblast-immune interactions. We will use genetic manipulation studies within these systems alongside transgenic mouse models to manipulate CAFs towards an autoimmune-like state and assess how this influences tumour growth and the immune landscape within the tumour.
Junior Group Leader Dermal Oncoimmunology
Dr. Hafsa Munir
 D. Jung
D. Jung
[since 2023] Junior Group Leader HI-TRON Mainz
[2021 – 2023] Postdoctoral Fellow at the Hospital for Special Surgery/Weill Cornell Medicine, USA
[2016 – 2021] Postdoctoral Fellow at the MRC Cancer Unit at the University of Cambridge, UK
[2012 – 2016] PhD at the Institute for Biomedical Research at the University of Birmingham, UK
[2019] Best talk prize at the annual Trinity College Forum, University of Cambridge
[2018] Best talk prize at the annual MRC Cancer Unit/Hutchison retreat
[2014] 26th UK Adhesion Society Meeting best poster prize
[2014] Travel Award, University of Birmingham
HI-TRON Mainz DKFZ
AG Munir
Obere Zahlbacherstr. 63
Building 911
55131 Mainz
Team
Alexander Trinks
PhD Student
Ibone Thate Arrazola
Biological technical assistant
Selected publications
- Munir H, Jones JO, Janowitz T , Martins CP, Shields JD. Stromal-driven and Amyloid β-dependent induction of neutrophil extracellular traps modulates tumour growth. Nature Communications. 2021; 12(1):683
- Lakins MA, Gohrani E, Munir H, Martins CP, Shields JD. Cancer-associated fibroblasts induce antigen-specific deletion of CD8 + T Cells to protect tumour cells. Nature Communications. 2018; 9(1):948
- Munir H, Clarke L, Sheriff L, Nash GB Mc Gettrick H. Adipogenic Differentiation of Mesenchymal Stem Cells Alters Their Immunomodulatory Properties in a Tissue-Specific Manner. Stem Cells. 2017; 35(6):1636-1646
- Munir H, Nash GB, Mc Gettrick HM Comparative Ability of Mesenchymal Stromal Cells from Different Tissues to Limit Neutrophil Recruitment to Inflamed Endothelium. PLOS ONE. 2016; 11(5):e0155161
Lab News
01/2024: A new members joins the Munir lab: Ibone Thate Arrazola
11/2023: A new members joins the Munir lab: Alexander Trinks